  
On the contrary, in ARDS the inhomogeneous damage to the alveolo-capillary membrane generates an exudative edema. 
Therefore, the thickening of the individual septum is limited by its own physical capacitance and when it is maximally distended (interstitial tamponade) alveolar flooding occurs ( 9). 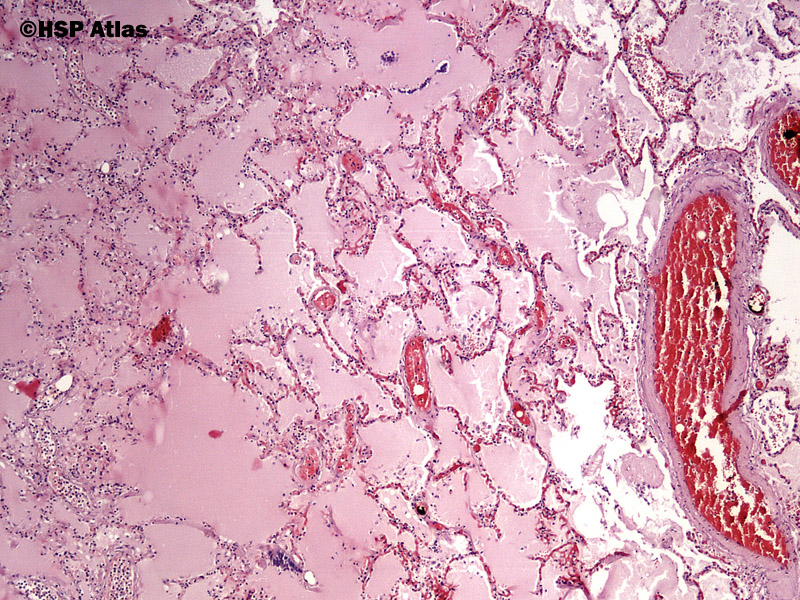
What is more interesting from an ultrasonographic and diagnostic point of view, is that in CPE fluid expands the secondary interlobular septa in a deterministic fashion, which is mainly related to a pressure gradient. This effect facilitates the peripheral clearance of the fluid toward the center of the lungs ( 8), and represents a valid compensatory mechanism which prevents alveolar flooding. The ongoing edema progressively expands and dilutes the extravascular fluid compartment around the vessels where the edema is taking place, creating an osmotic pressure gradient directed from the periphery to the center of the lung, where the osmotic pressure is higher. This space is continuous without interruptions with the interlobular septa and the subpleural tissue. In CPE, the first site of accumulation of extravascular lung water (a plasma ultrafiltrate) is in the loose connective tissue surrounding the blood vessels and bronchi. Moreover, in ARDS the heart can be normal in size, pulmonary and intrathoracic blood volume is not increased, and Kerley B-lines and peribronchial/perivascular cuffing are rare ( 7). Its distribution is frequently peripheral, patchy and non-gravitational. The accumulation of perivascular and intra-alveolar fluid increases lung weight, whereas patients who develop cellular proliferation fibrosis and type 2 pneumocyte hyperplasia show an anatomical remodelling of the lung, reduction in pulmonary compliance (stiff lung), worsening in gas exchange and increased mortality.Ĭlassical teaching states that capillary permeability edema is distinctive in chest X-rays and, mostly, in CTs. The histopathological features of ARDS follow three overlapping phases: an inflammatory phase with exudation of a protein rich fluid, a proliferative and cellular phase (often after only 72 hours) and a fibrogenic phase. The main characteristic of ARDS is the damage to the alveolar-capillary membrane which results in the accumulation of protein-rich fluid inside the alveolar septa and inside the alveoli ( 6). Therefore, in current practice ARDS is usually differentiated from CPE by the clinical picture and by physical findings, and this distinction is often completed by the response to therapy. Nowadays, patients are presumed to have ARDS if they show respiratory distress which cannot be explained by findings of heart failure or fluid overload on a clinical basis and by using all the available data, because the pulmonary capillary wedge pressure measurement has been removed from this definition. The Berlin definition for ARDS ( 4) shows a better predictive power for mortality than the previous ARDS definition by the American-European Consensus Conference (AECC) ( 5), but it includes potential differential diagnostic inconsistencies, mainly related to the poor sensitivity and specificity of the chest radiographic criteria for distinguishing ARDS from CPE. Moreover, in septic patients with ARDS, the myocardium is dysfunctional due to systemic inflammatory activation and mitochondrial impairment, and sepsis related cardiomyopathy ( 3) is a recognized cause of left ventricular failure and of an increase in hydrostatic extravascular lung water and CPE. This diagnostic task becomes more difficult in older patients, where a higher number of morbidities often coexists. Differentiating between hydrostatic or cardiogenic pulmonary edema (CPE) and ARDS is challenging, especially in the early stages of illness ( 2). Since its first description in 1967 ( 1), acute respiratory distress syndrome (ARDS) represents a well known major clinical problem in intensive care units (ICUs), carrying a high morbidity and mortality. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
